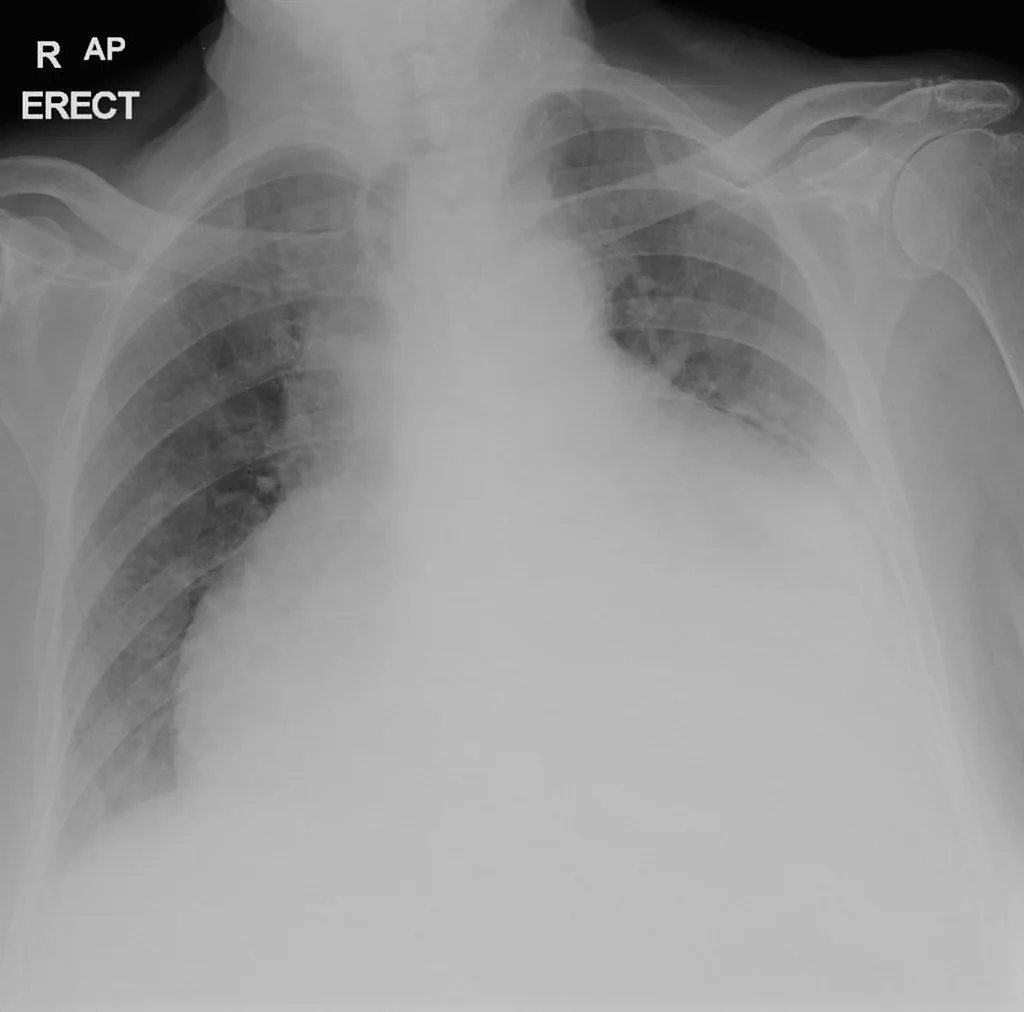
Definition
Accumulation of fluid in the space between parietal and visceral pericardium.
Causes of Pericardial Effusion
• After acute pericarditis (bacterial, viral).
• Tuberculosis (most common).
• Collagen diseases (SLE, rheumatoid arthritis)
• Myxoedema.
• Lymphoma.
• Neoplasm (secondary from carcinoma of breast, bronchial carcinoma).
• Renal failure and dialysis.
• After radiotherapy.
Clinical Features of Pericardial Effusion
Symptoms
• Heaviness in the chest or breathlessness.
• Palpitation.
• Symptoms of the primary cause.
Signs
1. Pulse—low volume, tachycardia, there may be pulsus paradoxus (indicating cardiac tamponade).
2. JVP—raised, Kussmaul’s sign positive (rise of JVP during inspiration. Normally, JVP falls
during inspiration).
3. Blood pressure—low systolic, normal diastolic, and narrow pulse pressure.
4. Precordium—
–– Area of cardiac dullness is increased (on percussion).
–– Apex beat is difficult to palpate. If palpable, it is within the area of cardiac dullness.
–– Heart sounds are muffled or distant.
–– Bronchial sound at the left inferior angle of the scapula (Ewart’s sign).
5. Liver is enlarged and tender.
Investigations
1. Chest X-ray—heart is enlarged, globular, pear-or pitcher- shaped with clear margin. Lung fields are oligaemic.
2. CBC (ESR high in tuberculosis, SLE, RA).
3. ECG (low-voltage tracing, tachycardia).
4. Echocardiogram (shows echo-free zone).
5. Paracentesis—see the colour, analysis of the pericardial fluid (Gram staining, AFB staining,
C/S, viral study, cytology, biochemistry).
6. Magnetic resonance imaging (MRI) is very helpful.
7. Other investigations according to the suspicion of causes—
–– TB (MT, sputum for AFB).
–– Collagen disease (RA test, ANA, Anti-ds-DNA).
–– Hypothyroidism (FT3, FT4, TSH).
Confirmation of Diagnosis
By echocardiogram (shows the echo-free zone). Paracentesis is definitive.
Treatment of Pericardial Effusion
According to cause—
• If tuberculosis, antituberculosis drug plus prednisolone is given.
• If bacterial cause is suspected—broad-spectrum antibiotic.
• Other treatment of primary cause (e.g. hypothyroidism, SLE, RA, lymphoma).
• Paracentesis, if cardiac temponade develops.
What is Paracentesis?
It is a procedure, in which fluids are aspirated from body, usually from the abdomen for diagnostic and treatment purposes.