Definition
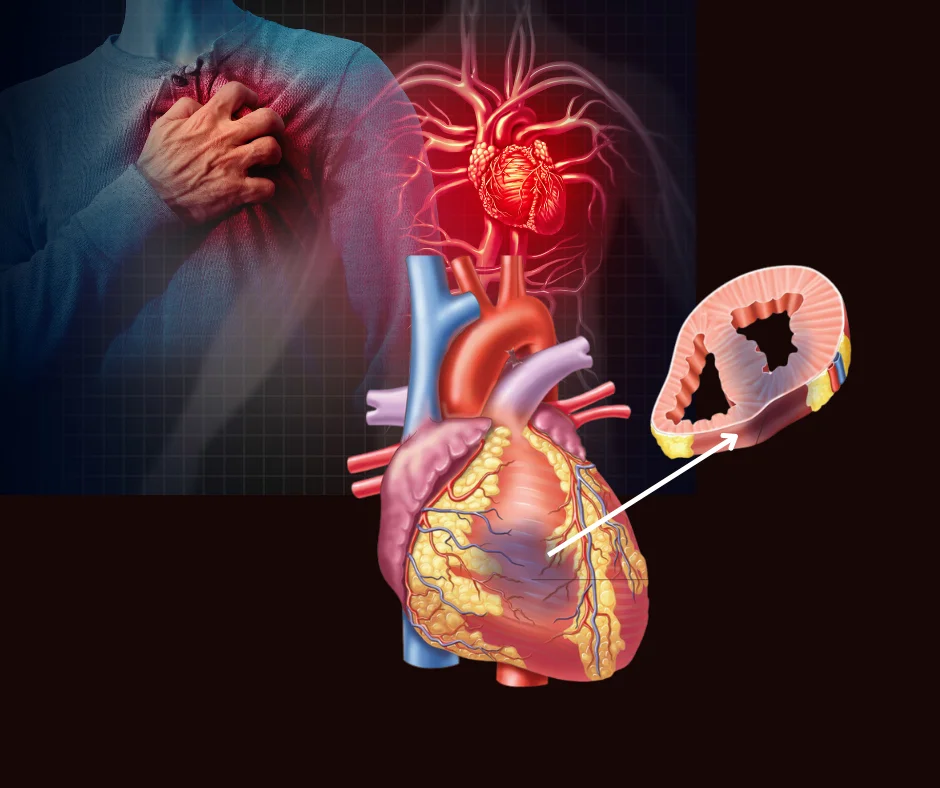
Heart attack or Myocardial infarction (MI) is defined as myocardial necrosis which occurs as a result of a critical imbalance between coronary blood flow and myocardial demand due to occlusion of the coronary artery by thrombus.
Types of MI
• Q-wave or ST-elevated or Transmural MI
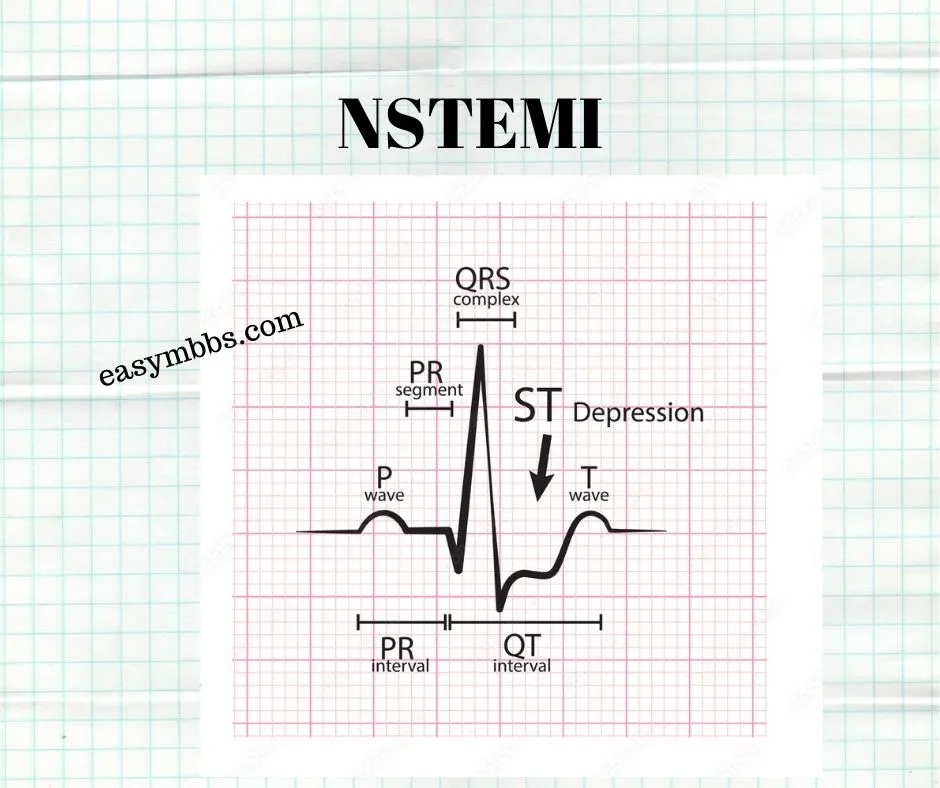
• Non-Q-wave or non-ST-elevated (NSTEMI) or subendocardial MI.
Clinical Features
Symptoms
- Central chest pain – which is severe, stabbing or squeezing, or constricting, and radiates to the lower jaw, neck, and inner side of the left arm up to the finger, not relieved by rest and nitroglycerine, and usually persists for more than 30 minutes.
- Sweating.
- Fear of impending death.
- Nausea and vomiting (more in inferior MI).
- Breathlessness.
- Collapse or cardiogenic shock.
Signs
- The patient is restless with pallor, sweating, and tachycardia (bradycardia in inferior MI).
- Hypotension, oliguria, cold peripheries.
- Signs of complications, e.g. cardiogenic shock, acute left ventricular failure, arrhythmia, mitral regurgitation, pericarditis.
Investigations
1. ECG shows—
–– ST-elevation (with upward convexity).
–– Pathological Q-wave.
–– T-inversion.
2. Enzymatic changes in acute MI—
–– Troponin I—rise in 2–4 hours, which may persist up to 7 days.
–– CPK—rise in 4–6 hours, and peak in 12 hours, but returns to normal within 48–72 hours. CK-MB is cardiac-specific.
–– SGOT—increases after 12 hours, and peaks in 24 hours, but returns to normal in 3–4 days.
–– LDH—rises after 12 hours, and peaks in 3–4 days, but is normal after 7–10 days.
3. Others—Chest X-ray, and echocardiography may be done.
/*! elementor – v3.6.5 – 27-04-2022 */
.elementor-widget-image{text-align:center}.elementor-widget-image a{display:inline-block}.elementor-widget-image a img[src$=”.svg”]{width:48px}.elementor-widget-image img{vertical-align:middle;display:inline-block} 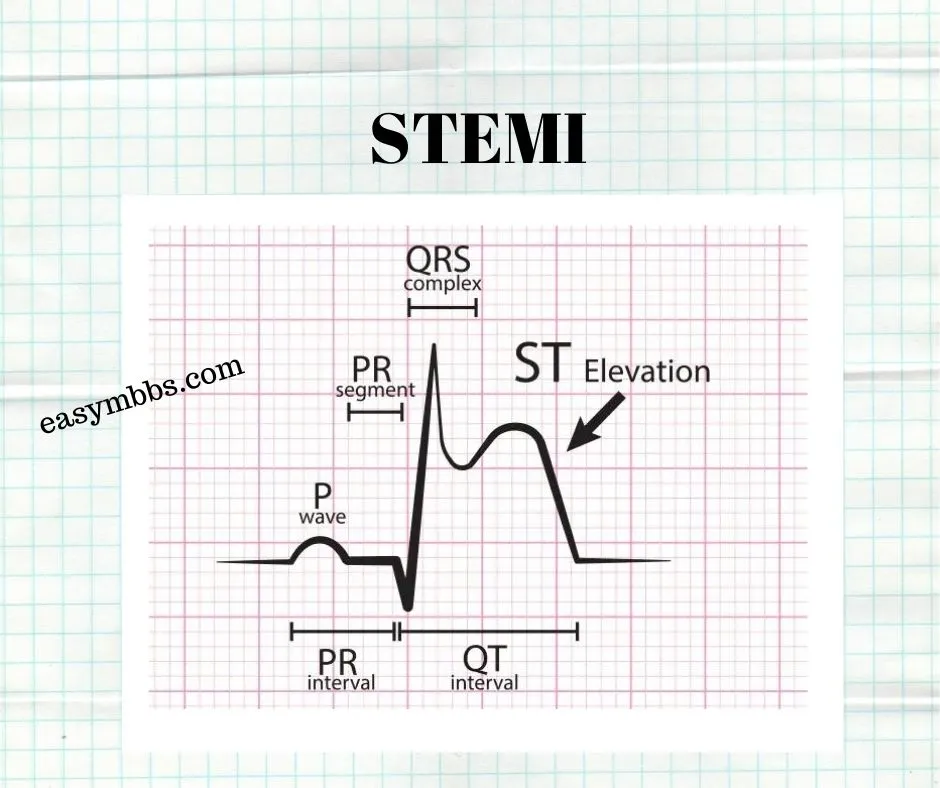
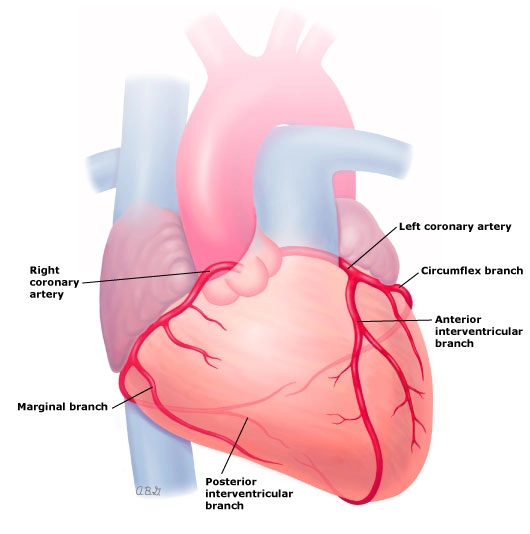
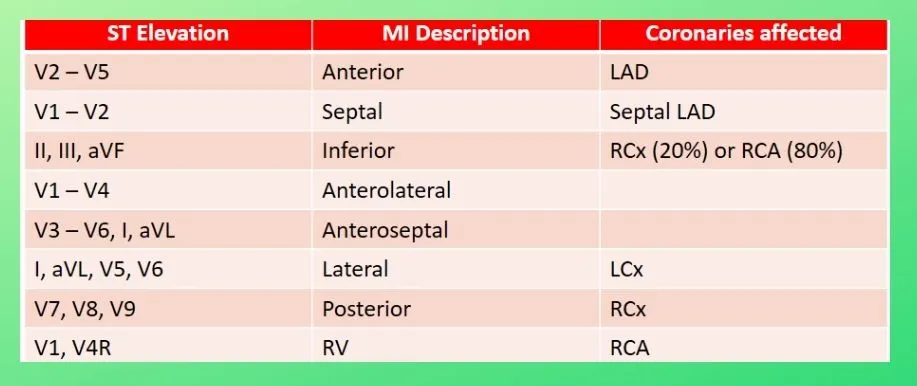
Sites of MI
• Inferior myocardial infarction.
• Anterior myocardial infarction.
• Anteroseptal myocardial infarction.
• Lateral myocardial infarction.
• Posterior (true) myocardial infarction.
• Subendocardial myocardial infarction.
Complications of Heart Attack or MI
It may be early or late:
1. Early complications—
–– Arrhythmia—Ventricular ectopics (more common), ventricular fibrillation, ventricular tachycardia, sinus bradycardia (common in inferior MI), sinus tachycardia, atrial fibrillation, heart block.
–– Cardiogenic shock.
–– Cardiac failure (LVF, biventricular failure).
–– Acute pericarditis (common in the 2nd or 3rd day).
–– Thromboembolism (systemic and pulmonary).
–– Rupture of papillary muscle or chordae tendineae resulting in MR.
–– Rupture of interventricular septum causing VSD.
–– Rupture of the ventricular wall.
2. Late complications—
–– Ventricular aneurysm (10%).
–– Postmyocardial infarction syndrome (Dressler’s syndrome).
–– Frozen shoulder.
–– Post-infarct angina (may occur in up to 50% of patients).
Treatment of Heart Attack or Acute Myocardial Infarction
• Admission to CCU.
• Complete bed rest.
• High-flow O2 inhalation (60%)—2–4 L/min by nasal cannula.
• To relieve pain—Inject morphine (5–10 mg) or diamorphine (2.5–5 mg) plus antiemetic (cyclizine or metoclopramide) IV. May be repeated, if necessary.
• Chewable aspirin—300 mg and clopidogrel 300 mg.
• Primary PCI, if available—treatment of choice. Should be performed as early as possible.
• Or thrombolytic therapy—streptokinase, if no contraindication.
• Other therapy—β-blocker (if no contraindication)—IV bolus atenolol 5–10 mg or metoprolol 5–15 mg slowly over 5 minutes. Oral atenolol 25–50 mg BD, or bisoprolol 5 mg daily or metoprolol 25–50 mg BD or TDS may be given.
• Sublingual nitroglycerin—0.3–1 mg.
• Anticoagulants—Heparin 5000 IU IV bolus, then 0.25 U/Kg/hour. Or low molecular weight heparin (S/C enoxaparin 1 mg/kg body weight 12 hourly.
• ACE inhibitor.
Criteria of thrombolytic therapy
• Typical history of chest pain.
• ECG change—ST-elevation > 1 mm in limb leads or 2 mm in chest leads (in 2 or more contiguous
leads) or new left bundle branch block.
• High cardiac enzyme.
===
Transmural: Passing through the wall of heart muscle.